What Patients Actually Need to Know Before They Show Up (Hint: It’s Not Just Clinical)
- John (JD) Donnelly

- 2 days ago
- 4 min read
For Community Health Centers, the mission has always been clear: deliver accessible, high-quality care to the communities that need it most.
But there’s a gap in how patients experience that mission.
Before a patient ever steps into an exam room, before vitals are taken or symptoms discussed, they’re asking a different set of questions:
Will my insurance cover this?
How much is this going to cost me?
Can I afford to follow through with care?
And too often, the system doesn’t have clear answers.
The Reality: Patients Are Making Decisions Before the Visit
Healthcare leaders often think of the patient journey as beginning at the point of care.
In reality, it starts much earlier.
Research shows that 9 in 10 patients want to know their financial responsibility before receiving care, and uncertainty around cost is a leading reason patients delay or avoid treatment altogether. Experian recently ranked “understanding the cost of care” among the top challenges for surveyed patients.
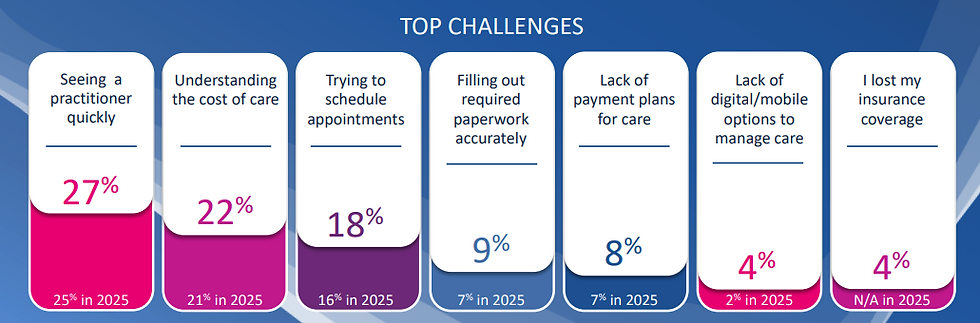
Similarly, a KFF (Kaiser Family Foundation) report found that a significant portion of adults, especially those with lower incomes, have postponed care due to cost concerns, even when insured.
For CHCs, this is especially critical. The populations they serve are disproportionately impacted by:
Medicaid complexity
Coverage variability
Sliding scale eligibility
Out-of-pocket sensitivity
When financial clarity is missing, patients hesitate, cancel, or fail to show up at all.
The Front-End Breakdown No One Talks About
Most CHCs have built strong clinical workflows. The care delivery model is thoughtful, coordinated, and patient-centered.
The financial experience? It’s often fragmented.
At the earliest touchpoints, teams are working with:
Incomplete or outdated eligibility data
Manual verification processes
Limited visibility into benefits and patient responsibility
Disconnected systems that don’t communicate in real time
Front-end inaccuracies like eligibility errors and incomplete patient information are among the top contributors to downstream claim denials and rework.
Patients are left navigating uncertainty at the exact moment they’re deciding whether to engage with care.
What Patients Actually Need (And Rarely Get)
If you strip it down, patients aren’t asking for perfection. They’re asking for clarity, and that shouldn’t be to much to ask for when it comes to a person’s health.
Before they show up, they need:
1. Confidence in Coverage
Not “we’ll check later.” Not “we think you’re covered.” Patients need (and deserve) real-time, reliable answers about whether their insurance applies to the visit.
2. A Clear Sense of Cost
Even an estimate changes behavior. Without it, patients are forced to assume the worst or delay care until they feel financially prepared.
3. Understanding of Their Options
For CHCs, this includes:
Sliding scale eligibility
Medicaid nuances
Self-pay pathways
Patients need to know what’s available to them, not discover it after the fact.
4. A Frictionless Experience
They shouldn’t have to repeat information, chase answers, or navigate multiple touchpoints just to understand basic financial details.
The Shift: From Clinical Readiness to Financial Readiness
For years, healthcare has optimized for clinical readiness. Of course, this is important, but patients are making decisions based on financial readiness.
The organizations that are leading right now are those that recognize:
A visit isn’t truly “scheduled” until it’s financially understood.
That means:
Eligibility verified in real-time, not overnight
Benefits clearly interpreted, not just retrieved
Patient responsibility is estimated before arrival
Financial pathways explained upfront
This is about removing the manual burden and replacing it with systems that provide clarity at the first point of contact. It’s not about creating more manual work for a typically short-staffed team.
Community Health Centers are already built around the patient. The task is to broaden this philosophy from the clinical to the financial experience.
When patients know what to expect:
They show up
They engage in care
They follow through on treatment
And when that happens, the impact compounds:
Stronger outcomes
More predictable revenue
Less strain on staff
Greater trust in the system
The Start of the Patient Journey
The patient journey begins in a moment of uncertainty, often with vulnerability surrounding one’s health and financial situation. That’s already a lot of stress.
Patients know care is available, but they don’t know if it’s accessible.
For CHCs, solving this must start before the visit, by ensuring every patient has the clarity, confidence, and information they need to move forward. Only when patients understand their financial reality are they far more likely to engage in their clinical care.
***
At FrontRunnerHC, we help Community Health Centers bring clarity to the very start of the patient journey. By delivering real-time eligibility, accurate benefits insight, and patient-friendly cost visibility at the first point of contact, we ensure patients understand their financial reality before they ever walk through the door. The result is simple: fewer surprises, stronger trust, better engagement, and a more sustainable path forward for the communities CHCs serve.
Frequently Asked Questions
What is a Community Health Center (CHC)?
A Community Health Center (CHC) is a community-based healthcare provider that delivers primary care and preventive services to underserved populations, regardless of a patient’s ability to pay. Many CHCs operate as Federally Qualified Health Centers (FQHCs) and offer services such as medical, dental, and behavioral health, often supported by sliding fee scale programs to ensure access for low-income patients.
How do Community Health Centers verify patient insurance eligibility?
Community Health Centers verify patient insurance eligibility by submitting electronic 270/271 transactions to payers, which return coverage details, including active insurance status, benefits, and patient responsibility. Many CHCs still rely on manual or batch eligibility checks, but real-time eligibility verification is becoming increasingly important to improve accuracy, reduce claim denials, and provide patients with upfront financial clarity.
Why is cost transparency important for patients at Community Health Centers?
Cost transparency is critical at Community Health Centers because many patients face financial uncertainty and may delay or avoid care without clear information about what they will owe. Providing upfront estimates, explaining sliding-scale discounts, and confirming coverage before the visit help patients make informed decisions, improve appointment adherence, and support better health and financial outcomes for both patients and the health center.




Comments